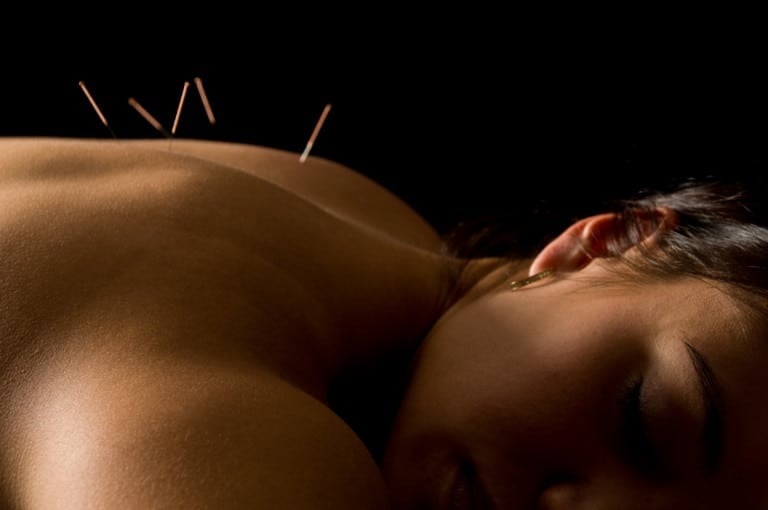
Real Richmond Patients Share What Actually Changed: Acupuncture for Anxiety Success Stories
How Acupuncture and Chinese Medicine Actually Help Anxiety
If you’re reading this, you’ve probably already tried things for your anxiety. Maybe therapy. Maybe medication. Maybe both. And maybe they helped — but didn’t get you all the way there.
As a licensed acupuncturist in Richmond, Virginia who specializes in complex, multi-system conditions, I work with patients like you every week. And the reason acupuncture and Chinese medicine succeed where other approaches fall short usually comes down to two things.
First, acupuncture is one of the most effective tools we have for rebalancing a dysregulated nervous system. Your autonomic nervous system controls your stress response, your heart rate, your digestion, your sleep — all the things that go haywire when anxiety takes hold. When that system gets stuck in sympathetic overdrive (fight-or-flight mode), your body produces anxiety symptoms even when there’s nothing to be anxious about. Acupuncture directly calms that response, and research consistently shows it works — multiple 2025 systematic reviews confirm that acupuncture produces clinically significant reductions in anxiety.
Second, Chinese medicine doesn’t treat anxiety as one condition. It recognizes that anxiety has multiple distinct root causes — and each one requires a different treatment strategy. Some patients have a blood circulation issue. Others have gut inflammation disrupting their brain chemistry. Others have a hormonal pattern that amplifies anxiety at specific times of the month. Identifying the right root cause is what makes the difference between temporary relief and lasting change. (I go deep on the six Chinese medicine patterns behind anxiety here if you want the full picture.)
And when the root cause is complex — involving autoimmune issues, digestive dysfunction, or hormonal imbalances — I often combine acupuncture with Chinese herbal medicine to stabilize results between visits. Keep reading past the success stories below, and I’ll explain exactly when acupuncture works powerfully on its own versus when herbs become an important part of the equation.
But first — the stories. Because these acupuncture for anxiety success stories from my practice are the best way I know to show you what’s possible.
Acupuncture for Anxiety Success Stories From My Practice
A note about these stories: To protect patient privacy, I’ve changed identifying details like names and ages. But the symptoms, timelines, and outcomes are real — drawn from patients I’ve treated here in Richmond. These aren’t hypothetical examples or composites from a textbook. They’re what actually happens in my clinic.
Danielle, Early 30s: “My Stress Used to Take Over My Entire Body — 95% of That Is Gone”
Where she started:
Danielle didn’t come in for anxiety specifically — she came in because stress had taken over her body and she couldn’t get it to stop. She described herself as someone who internalizes everything and holds onto it for a long time. Years of high-stress work environments had worn down her ability to cope, and more recently, even moderate stressors were overwhelming her system.
When stress hit, it wasn’t just mental — it was intensely physical. She’d feel tension rising from her chest up through her neck and into her head. She’d become overstimulated to the point where she couldn’t process what was happening around her. She’d clench her jaw. She’d get short-tempered. Her stress baseline sat around a 4 out of 10 on calm days, but during demanding periods it would spike to a 7 or 8. She described her stress resilience as poor — she noticed that peers in similar situations seemed to handle things more easily.
On top of the stress and anxiety, Danielle was dealing with a chronic skin condition that had plagued her for years and had worsened significantly under stress. The flare-ups were so severe that they limited her ability to exercise (heat and sweat triggered them), which trapped her in a cycle of inactivity and worsening stress. She’d tried seemingly everything — dietary changes, medications, cold showers — with limited relief.
She found our clinic through the website and came in looking for, in her words, “another tool in my toolbox for stopping spirals and creating a routine of wellness.” She told me she believed her issues had long been stored in her body. She was right.
What I found:
Danielle’s case was a clear example of how chronic, internalized stress disrupts the body from the inside out. Her nervous system had been running in overdrive for years, and the physical symptoms — the chest-to-head tension, the jaw clenching, the skin flare-ups, the overstimulation — were all signs that her body’s stress response was stuck on high and had nowhere to go. The stress wasn’t just making her feel bad; it was creating real inflammation and physical dysfunction.
The treatment plan:
We started with acupuncture twice a week for five weeks — no herbs in this case, partly because of timing with her other medical treatments. The focus was on calming and resetting her nervous system, releasing the physical tension patterns that had built up over years, and improving her body’s ability to shift out of fight-or-flight mode.
Timeline of changes:
- First 2 weeks: Danielle noticed she was less reactive to daily stressors. The chest-to-head tension pattern was loosening. She was sleeping more soundly.
- 1 month: The overstimulation episodes — where she’d shut down and couldn’t process anything — were becoming rare. Her baseline stress level was dropping noticeably. She reported feeling more like herself than she had in a long time.
- 3 months: 95% resolution. The stress and anxiety that had dominated her body were essentially gone. The physical tension pattern that used to climb from her chest to her head had resolved. Her jaw clenching decreased dramatically. Her skin condition — which had been flaring in direct response to her stress levels — improved significantly as her nervous system calmed down.
Where she is now:
Danielle’s case is one of my favorites to share because it shows something important: when the primary driver of your symptoms is a dysregulated nervous system, acupuncture alone can produce dramatic results. She didn’t need herbs. She didn’t need a complicated protocol. She needed her nervous system to come out of crisis mode — and once it did, her body started healing across the board. The skin issues, the tension, the reactivity, the feeling of being overwhelmed — all of it improved together because it all had the same root cause.
Rachel, Early 30s: “I Haven’t Had a Panic Attack in Over a Week — That Hasn’t Happened in Months”
Where she started:
Rachel came to me after a traumatic event turned her life upside down, and even though months had passed, her body was still stuck in crisis mode. She was waking up two to three nights a week in a full panic attack — heart pounding, drenched in sweat, unable to fall back asleep for hours. On a good night she was getting six hours of broken sleep. On a bad night, four.
She’d been in talk therapy on and off for years and was still going, but she put it to me plainly: “Intellectually, I feel more healed. But my body hasn’t caught up.” The panic attacks had no identifiable trigger — they would just jolt her awake. She was exhausted, struggling to concentrate during the day, and had started dreading going to bed at night.
On top of the PTSD symptoms, Rachel had a long history of hormonal and digestive issues — thyroid problems, weight management challenges despite a healthy lifestyle, chronic constipation, and food sensitivities that had developed after a severe allergic reaction years earlier. She was on several medications for her endocrine issues, and while those had helped stabilize some of her symptoms, the anxiety and sleep disruption were getting worse, not better.
What I found:
Rachel’s case was a textbook example of why anxiety is so often a whole-body problem. Her nervous system was locked in sympathetic overdrive from the trauma, but it wasn’t operating in a vacuum — it was layered on top of years of endocrine disruption, digestive inflammation, and chronic sleep deprivation. Each of those systems was making the others worse. The panic attacks weren’t just “in her head.” Her body had real, physical reasons to be sounding alarm bells.
The treatment plan:
We started with acupuncture twice a week for five weeks, focused on calming the nervous system and addressing the underlying patterns I identified. No herbs initially — I wanted to see how her body responded to acupuncture alone first, given the medications she was already taking.
Timeline of changes:
- First 2 weeks: Rachel reported a 30% improvement. The biggest change? She went a full week without a single panic attack — something that hadn’t happened in months. Her sleep wasn’t perfect yet, but the night-waking episodes were less intense when they did happen.
- 1 month: [MAEGAN TO UPDATE as treatment progresses]
- 3 months: [MAEGAN TO UPDATE as treatment progresses]
Where she is now:
Rachel is still early in her treatment — this is a story that’s being written in real time. But the fact that she saw meaningful improvement in just two weeks of acupuncture, with no herbal medicine and no changes to her existing medications, tells me her body was ready to respond once it got the right support. I’ll update this story as her treatment progresses.
Mia, Late 20s: “I’m 80% Better — The Panic Attacks That Used to Happen Every Week Are Almost Gone”
Where she started:
Mia’s anxiety didn’t just live in her head — it took over her entire body. At baseline, she rated her anxiety a 5 out of 10, but it would spike to 7 or higher during stressful periods. She was having about one panic attack a week, and her panic attacks weren’t ordinary — they would cause her blood pressure to drop, her limbs to go numb, and sometimes she’d faint. She’d passed out in public more than once. She was getting close to fainting at least once a month.
The anxiety showed up as OCD-like behaviors (compulsive cleaning, repetitive checking), constant tension headaches, stomach pain around her navel, nausea during panic episodes, and worsening asthma and coughing. She was fatigued nearly all the time, easily frustrated, and her mood was suffering. Before her period, everything amplified — the anxiety, the anger, the shaking, the feeling of being ice cold.
She’d been doing “all the wellness things” on her own but couldn’t get ahead of it. Her digestion was unreliable — alternating between constipation and stress-triggered loose stools. She had food sensitivities, frequent urinary tract infections, and was always cold. She found our clinic through reviews and came in hoping for real relief.
What I found:
Mia had several patterns layered together, which is common in complex anxiety cases. The digestive symptoms, fatigue, cold sensitivity, and the way stress immediately disrupted her gut pointed to significant digestive weakness that was failing to nourish the rest of her body properly. On top of that, there was a pattern of pent-up heat and tension — the headaches, the irritability, the acne that flared with stress, and the way her anxiety would build until it literally knocked her off her feet. Her body was simultaneously depleted and overheated, which is one of the trickiest combinations to treat — and one of the reasons herbs were essential from the beginning.
The treatment plan:
Mia started with acupuncture and Chinese herbal medicine together from day one. This was a case where I knew acupuncture alone wouldn’t be enough — there was too much going on between her digestive dysfunction, the hormonal component, and the severity of her physical anxiety symptoms. The herbs needed to work between visits to address the gut issues and calm the inflammatory patterns that were feeding her anxiety.
One thing that’s important to understand about Chinese herbal medicine: the formula often changes as the patient changes. Mia didn’t stay on the same herbs the whole time. I started with formulas targeting her digestive weakness and the pent-up stress pattern. As her digestion stabilized and some of the surface-level tension cleared, I was able to shift the herbal strategy to address deeper patterns — including the heat and inflammation that were driving her headaches, skin breakouts, and the intensity of her panic episodes. This kind of adjustment is why working with an experienced practitioner matters — the herbs need to evolve with you.
Timeline of changes:
- 2 weeks: Mia appeared noticeably calmer at her follow-up. She missed a dose of her regular medication and — for the first time — didn’t have a panic attack. She rated her anxiety as 40% better, dropping from her usual 5 out of 10 to about a 3.
- 1 month: She reported feeling 70% better overall. Her bowel movements had regulated to daily. Anxiety was sitting around a 1.5 out of 10 on most days.
- 6 weeks: 80% better. What used to be a constant 5 out of 10 anxiety baseline was now hovering around a 1. The panic attacks that had been happening weekly were now rare.
- 3 months: Holding steady. Her concentration had improved (with help from a new medication her doctor prescribed). Fatigue was still present but significantly better. The fainting episodes that used to happen monthly had stopped.
Where she is now:
The numbers speak for themselves: 80% improvement from where she started. The anxiety that used to dominate her life — the fainting, the OCD-like symptoms, the weekly panic attacks — has become manageable. She’s sleeping, she’s eating better, her digestion has regulated, and the fainting episodes have stopped. She told me recently that she believes she can fully heal. That shift in itself is huge.
Jess, Mid 20s: “I Used to Convince Myself Something Was Seriously Wrong With Me Every Single Day — Now My Anxiety Is 80% Gone”
Where she started:
Jess came in overwhelmed and scared. Her primary issue was health anxiety — a relentless cycle of noticing a physical sensation, Googling it, and spiraling into panic that something was seriously wrong. “I can create the pain in a way,” she told me during her first visit. She knew intellectually that her fears weren’t rational — her bloodwork and physical were normal — but her body wouldn’t stop sounding the alarm.
At the time, she was experiencing muscle weakness and fatigue that came and went with her anxiety levels, night sweats that were disrupting her sleep, palpitations and chest tightness, a constant bad taste in her mouth, loose stools, low appetite, and a deep feeling of being “not herself.” She cried easily, was constantly tense, and was easily startled. She was on an SSRI for the anxiety but felt it wasn’t enough.
The thing that struck me most was what she said at the end of her intake: “I am scared I will always feel this way.” That’s a sentence I hear often from anxiety patients, and it always tells me two things — they’re suffering, and they’re ready for something to actually work.
What I found:
Jess had two distinct patterns happening simultaneously, which is why treating her anxiety required a phased approach.
The first pattern involved excess heat and stagnation — pent-up stress and tension that was generating the night sweats, palpitations, chest tightness, the bad taste in her mouth, and the easily-startled nervous system. Her body was running hot and tight. This needed to be cleared first before we could build anything up.
The second pattern, sitting underneath the first, was a deeper deficiency — her digestive system and heart energy were depleted. This is what was causing the fatigue, the muscle weakness, the low appetite, the loose stools, and the way her body simply didn’t have the resources to calm itself down. You can think of it like a bank account that’s been overdrawn — until you address the deficit, the overdraft fees (anxiety symptoms) just keep piling up.
The treatment plan:
Jess started on weekly acupuncture sessions combined with Chinese herbal medicine from the beginning. This is a case where the herbs were essential — acupuncture could calm her nervous system in the moment, but the herbs needed to work between visits to address both the heat pattern and the underlying deficiency.
The herbal strategy shifted as Jess improved. In the first phase, I prescribed formulas to clear the excess heat and move the stuck energy — targeting the night sweats, chest tension, and the agitated, easily-startled quality of her anxiety. As those symptoms cleared, I transitioned to formulas that focused on strengthening her digestion and nourishing her heart energy — rebuilding the foundation that had been depleted. This two-phase approach is common in my practice: you clear what’s excess first, then build what’s deficient. Doing it in the wrong order can actually make things worse.
Timeline of changes:
- First 2 weeks: The night sweats improved quickly. She was no longer waking up hot. The shortness of breath she’d been experiencing resolved. Her appetite started to return.
- 1 month: The bad taste in her mouth was gone. Sleep was improving. She was less easily startled, and the chest tightness was easing. The muscle weakness — the symptom that had sent her spiraling in the first place — was fading as her anxiety decreased.
- 3 months: 80% improvement. At a follow-up, she reported that her anxiety had been “good” — a word she couldn’t have imagined using three months earlier. The night sweats were gone. The palpitations had stopped. Her appetite and digestion had normalized. She was sleeping through the night. The health anxiety spirals that used to consume her daily were now rare and manageable.
Where she is now:
Jess continued with maintenance visits after her initial treatment course. By that point, anxiety was no longer her primary concern at appointments — she’d shifted to working on residual neck and shoulder tension, which is a common and welcome sign that the deeper issues have resolved. The woman who walked in terrified she’d always feel that way had become someone who barely thought about anxiety most days.
Tom, Late 60s: “I Had My First Panic Attack at 67 Years Old — Ten Sessions Later, I Got My Life Back”
Where he started:
Tom had been a patient of mine on and off for years, coming in for various issues as they came up. So when he called to schedule an urgent appointment, I knew something was wrong. He’d had his first-ever panic attack — during a work meeting, in front of colleagues — and it shook him to his core. He’d never experienced anything like it.
What followed made it worse. Over the next week and a half, he was subjected to several traumatic events related to the initial incident. He was eventually diagnosed as Post-Traumatic Stress Disorder (PTSD). He got into therapy, which was helping him develop coping strategies. But his body was still in crisis. He came to me specifically for help rebalancing his nervous system.
What made Tom’s case different from most of my anxiety patients is that he had no prior history of anxiety or panic. This wasn’t a lifelong pattern — it was an acute trauma response in a man whose nervous system had been stable for decades. His body had been knocked out of equilibrium by a specific event, and it needed help finding its way back.
What I found:
Tom’s nervous system was stuck in a heightened state of vigilance — classic for PTSD. His vagus nerve, which is the main pathway for shifting from fight-or-flight into rest-and-repair mode, wasn’t doing its job. The panic attack had essentially flipped a switch, and his body didn’t know how to flip it back. Because he didn’t have underlying deficiencies or chronic health issues complicating the picture, this was a case where acupuncture could work quickly and directly.
The treatment plan:
Acupuncture only, focused on vagus nerve regulation and calming the sympathetic nervous system. No herbs needed — this was a clear-cut case of nervous system dysregulation without the layers of digestive, hormonal, or immune dysfunction that make other anxiety cases more complex.
Timeline of changes:
- After 5 visits: Tom’s baseline anxiety had dropped significantly. The hypervigilance was easing. He was no longer bracing for the next panic attack.
- After 10 visits: 85% improvement. The man who had walked in rattled by his first-ever panic attack was back to feeling like himself. The PTSD symptoms that had been dominating his daily life had largely resolved.
Where he is now:
Tom returned to the on-and-off maintenance pattern we’d had before — coming in as needed for other issues, with anxiety no longer a huge priority on the list. His case is a powerful reminder that acupuncture can be remarkably effective for acute trauma responses, especially when the person doesn’t have a long history of chronic health issues underneath. Sometimes, the nervous system just needs a skilled reset.
What If Your Anxiety Isn’t “Just Anxiety”?
The success stories above share something in common: in every case, the anxiety turned out to be connected to a physical issue that nobody had looked for. This is something I see constantly in my practice, and it’s worth understanding — because it might change how you think about your own anxiety.
Here’s something most doctors won’t tell you: anxiety is often a symptom of a physical problem that has nothing to do with your mental health. A patient comes in after years of therapy and medication that helped — but didn’t fully resolve their anxiety. When I start digging into the bigger picture, we often find something physical driving the bus. Things like:
- Histamine overload — when your body can’t break down histamine fast enough (often due to gut inflammation, Mast Cell Activation Syndrome (MCAS), or enzyme deficiencies), the excess histamine floods your nervous system. The result? Anxiety, racing heart, insomnia, and brain fog that look exactly like a psychiatric condition — but aren’t.
- Nutritional deficiencies — low magnesium, vitamin B12, iron, vitamin D, and zinc are all directly linked to anxiety and nervous system dysfunction. Magnesium alone is involved in over 300 biochemical reactions in your body, including the regulation of stress hormones. And studies suggest the majority of Americans aren’t getting enough.
- Gut-brain axis disruption — your gut produces many of the same neurotransmitters as your brain, including serotonin. When gut health is compromised — through dysbiosis, intestinal permeability, Small Intestinal Bacterial Overgrowth (SIBO), or chronic inflammation — the signaling between your gut and your brain breaks down. Anxiety is often the first symptom.
- Nervous system dysregulation — your autonomic nervous system controls everything from your heart rate to your digestion to your stress response. When it’s stuck in sympathetic overdrive (fight-or-flight mode), your body produces anxiety symptoms even when there’s nothing to be anxious about. This is one of the things acupuncture is exceptionally good at — rebalancing a dysregulated nervous system.
- Hormonal imbalances — thyroid dysfunction, estrogen dominance, and cortisol dysregulation from chronic stress can all produce or amplify anxiety. These conditions are common, frequently missed in standard workups, and highly treatable.
- Poor Blood circulation — when blood flow is impaired, your brain and heart don’t get the nourishment they need. The body compensates with adrenaline surges that mimic — or cause — panic attacks.
I’m not saying anxiety is never psychological. It can be. But in my experience treating anxiety patients here in Richmond, the root cause is physical far more often than people expect. And when you identify and treat the physical driver, the anxiety often resolves in ways that medication alone never achieved.
Why I Often Recommend Chinese Herbs Alongside Acupuncture for Anxiety
One thing I want to address directly, because patients ask about this a lot: acupuncture alone can absolutely help with anxiety. But in many cases — especially the more complex ones — I recommend combining acupuncture with Chinese herbal medicine for stronger, longer-lasting results.
Here’s why. Acupuncture is powerful at resetting your nervous system in the moment. It calms the sympathetic (fight-or-flight) response, improves circulation, and helps your body shift back into a state where healing can happen. But the effects of a single acupuncture session, particularly early in treatment, can be relatively short-lived — especially if your body has an ongoing physical issue that keeps re-triggering the anxiety.
Chinese herbal formulas work between your acupuncture visits. They provide continuous support to the body systems that are driving the anxiety, so each acupuncture session can build on the last rather than starting from scratch.
I tend to recommend herbs especially when a patient’s anxiety is layered with other significant health issues. A few common examples:
- Autoimmune conditions or MCAS — when the immune system is overactive and driving inflammation (including histamine overload), herbs can help stabilize the immune response and calm the inflammatory cascade that’s feeding the anxiety.
- Significant digestive problems — if a patient has IBS, SIBO, chronic bloating, or gut inflammation, the gut-brain axis is likely a major contributor to their anxiety. Herbal formulas can address the digestive dysfunction directly while acupuncture works on the nervous system from the other direction.
- Menstrual-related anxiety — when anxiety intensifies around specific phases of the menstrual cycle, it usually points to a hormonal component that benefits from herbal support. Herbs can help smooth out the hormonal fluctuations that are amplifying anxiety at certain times of the month.
These are just a few examples — every patient is different, and I make herbal recommendations based on the specific pattern I identify in each case. But the general principle is this: the more complex the picture, the more important herbs become for stabilizing the results.
Working with an experienced practitioner who can identify the right herbal formula for your specific presentation is critical. This isn’t a situation where a generic “calming supplement” from the drugstore will do the same thing. The precision of the formula — matching it to your exact pattern — is what makes the difference between something that sort of helps and something that actually changes the trajectory of your treatment.
Does Acupuncture Really Work for Anxiety? What the Research Shows
I understand the skepticism. “Needles for anxiety?” sounds counterintuitive. But the research supporting acupuncture for anxiety has grown substantially, and the results are encouraging.
A 2025 systematic review and meta-analysis in the Journal of Clinical Psychology (Jang et al.) evaluated randomized controlled trials comparing acupuncture to sham acupuncture and standard care for anxiety. The analysis found that acupuncture produced statistically significant reductions in anxiety symptoms compared to control groups (Jang et al., 2025).
Another 2025 systematic review in Annals of General Psychiatry focused specifically on GAD and included studies through August 2025. This review assessed both acupuncture as a standalone treatment and as an add-on to medication, finding benefits in both scenarios — particularly when acupuncture was combined with existing treatment protocols (Lai et al., 2025).
A separate 2025 meta-analysis in Frontiers in Neurology (Jiang et al.) compared real acupuncture to sham acupuncture specifically for GAD. The researchers found that acupuncture produced clinically relevant improvements — not just statistically significant ones — on validated anxiety scales, suggesting the benefits go beyond placebo (Jiang et al., 2025).
For patients who are currently taking medication and wondering if acupuncture can help alongside it — yes, research supports that too. A 2024 subgroup analysis from the large AcuSDep trial found that adding acupuncture to Selective Serotonin Reuptake Inhibitor (SSRI) treatment produced comprehensive improvements for patients with anxious depression, with effects on both anxiety and physical symptoms like sleep disturbance (Zhao et al., 2024).
A 2021 meta-analysis of 20 randomized controlled trials found that acupuncture was more effective than control conditions for reducing anxiety, with good tolerance and safety profiles — meaning patients tolerated acupuncture well and side effects were minimal (Li et al., 2021).
The bottom line: a growing body of evidence supports acupuncture as an effective treatment for anxiety — both on its own and alongside conventional approaches like medication and therapy.
A Note About Medication
I want to be clear about something: if you’re on medication for anxiety, that’s okay. Many of my patients are on SSRIs or other medications when they start treatment, and I never ask anyone to stop their medication. That’s a conversation between you and your prescribing doctor.
What I’ve seen in my practice — and what the research supports — is that acupuncture and herbal medicine can work alongside your existing treatment. Some patients eventually work with their doctors to reduce or come off medication as their symptoms improve. Others stay on their medication and use acupuncture to address symptoms that medication alone wasn’t fully resolving — like sleep disruption, digestive issues, or physical tension.
If you’re wondering about herb-drug interactions — yes, they do exist, though they’re rare. This is something I take seriously. Before prescribing any herbal formula, I review every medication you’re currently taking and only prescribe herbs that are known to work safely alongside them. It’s one of the reasons working with a trained practitioner matters — I’m not guessing about compatibility.
There’s no wrong path here. The goal is getting you to a place where anxiety isn’t running your life.
What Your First Visit Looks Like
If you’ve never tried acupuncture before, I know the idea of starting can feel like one more thing to be anxious about. So let me walk you through exactly what to expect.
Your first step is a complimentary consultation — a free visit where we sit down together and I learn about what you’re experiencing. There’s no treatment at this visit and no pressure. It’s a chance for me to understand your situation and for you to decide if this feels like the right fit.
If we move forward, your first treatment visit is where the real work begins. Before you arrive, I’ll have already studied your intake form in detail and worked up preliminary ideas about what’s driving your anxiety. I come prepared with targeted questions to clarify the diagnosis — the kind of questions that might seem unrelated (like asking about your digestion or whether your hands and feet run cold) but are actually essential clues.
At that visit, you’ll receive your first acupuncture treatment and your first herbal prescription. I’ll also give you a Symptom Tracker — a simple tool where you track things like sleep quality, digestion, and energy between visits. These early indicators tell us whether treatment is heading in the right direction, often before the anxiety itself starts to shift.
Ready to Write Your Own Success Story?
If you’re reading these acupuncture for anxiety success stories and thinking that sounds like me — I’d love to talk with you.
I offer a free new patient consultation where we can discuss your situation, what you’ve already tried, and whether my approach might be the missing piece. There’s no commitment and no pressure — just an honest conversation about what’s possible.
Centered Richmond Acupuncture & Wellness 20 N. 20th St., Suite A, Richmond, VA 23223 Phone: (804) 234-3843
I work with patients from across the Richmond area — the Fan District, Church Hill, Short Pump, Midlothian, Glen Allen, and beyond.
Schedule Your Free Consultation | Learn More About Starting Treatment
Related Articles
- Acupuncture for Anxiety: A Chinese Medicine Guide to 6 Types of Anxiety
- Acupuncture for Depression
- Acupuncture for Stress
- Chinese Herbal Medicine (TCM Herbal Biotherapy)
- Acupuncture for MCAS
References
Li, Q., et al. (2021). Effectiveness of acupuncture on anxiety disorder: a systematic review and meta-analysis of randomised controlled trials. Annals of General Psychiatry, 20, 9. https://link.springer.com/article/10.1186/s12991-021-00327-5
Jang, S., Zheng, S. (2025). Acupuncture for Anxiety: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Journal of Clinical Psychology, 82, 479–494. https://onlinelibrary.wiley.com/doi/10.1002/jclp.70079
Lai, J., Wang, Y., Yao, X. et al. (2025). Efficacy of acupuncture for generalized anxiety disorder: a systematic review. Annals of General Psychiatry, 24, 73. https://link.springer.com/article/10.1186/s12991-025-00614-5
Jiang, L., Ma, Y., Huang, X., Li, J., & Hao, Y. (2025). Efficacy of acupuncture versus sham acupuncture on generalized anxiety disorder: a meta-analysis of randomized controlled trials. Frontiers in Neurology, 16, 1682400. https://www.frontiersin.org/journals/neurology/articles/10.3389/fneur.2025.1682400
Zhao, B., Li, Z., Shi, C. et al. (2024). Acupuncture as Add-on Therapy to SSRIs Can Improve Outcomes of Treatment for Anxious Depression: Subgroup Analysis of the AcuSDep Trial. Neuropsychiatric Disease and Treatment, 20, 1049–1064. https://pmc.ncbi.nlm.nih.gov/articles/PMC11104384/